Healthcare organizations today are facing a growing challenge: delivering faster access to care while managing increasing patient volumes, operational complexity, and rising expectations for digital experiences.
At the center of this challenge lies one critical workflow - ambulatory appointment scheduling.
For many providers, scheduling is still handled through a combination of legacy systems, manual coordination, and disconnected tools. The result is a fragmented experience for both patients and care teams: long wait times, scheduling errors, inefficient resource utilization, and missed revenue opportunities.
This is where FHIR (Fast Healthcare Interoperability Resources) is fundamentally changing the way scheduling systems operate.
Rather than treating scheduling as a standalone administrative function, FHIR enables it to become a connected, real-time, and intelligent workflow, deeply integrated with clinical systems, patient engagement tools, and operational data.
Why Ambulatory Appointment Scheduling Still Needs Modernization

Ambulatory care settings are inherently dynamic. Unlike inpatient environments, they must accommodate:
- Multiple providers with varying schedules
- High patient turnover
- Different appointment types (consultations, follow-ups, diagnostics)
- Coordination across locations and departments
In traditional systems, these variables are managed through static scheduling tools that lack real-time synchronization.
The result is a series of systemic inefficiencies:
Patients often experience:
- Long wait times just to book appointments
- Limited visibility into available slots
- Difficulty rescheduling or canceling
Healthcare staff deal with:
- High call volumes
- Manual data entry
- Scheduling conflicts and double bookings
Leadership faces:
- Underutilized provider capacity
- High no-show rates
- Lack of visibility into scheduling performance
These challenges are not just operational - they directly affect patient satisfaction, care access, and financial performance.
What Makes FHIR Different from Legacy Healthcare Standards
To understand how FHIR improves scheduling, it’s important to look at how it differs from traditional healthcare integration standards like HL7 v2 or CDA.
Legacy systems were designed primarily for data exchange between internal hospital systems, not for modern, patient-facing digital experiences. They rely on:
- Batch-based data transfer
- Complex message structures
- Custom integrations that are difficult to scale
FHIR, on the other hand, is built using modern web technologies, which fundamentally changes how systems communicate.
Key architectural differences:
FHIR uses:
- RESTful APIs for real-time communication
- JSON/XML formats for lightweight data exchange
- Modular resources (like Appointment, Patient, Schedule)
This means that instead of waiting for systems to sync periodically, data is updated instantly, enabling real-time scheduling decisions.
From a developer perspective, FHIR behaves like a modern API ecosystem. From a business perspective, it enables faster, more responsive operations.
FHIR vs Traditional Integration: Why It Matters for Appointment Scheduling

To understand the true impact of FHIR on ambulatory scheduling, it’s important to compare it with traditional healthcare integration approaches such as HL7 v2 and CDA.
Legacy systems were built for internal data exchange, not for real-time, patient-facing workflows. As a result, they struggle to support modern scheduling needs like instant booking, dynamic updates, and seamless multi-system coordination.
FHIR changes this by introducing a real-time, API-driven architecture that aligns with how modern digital systems operate.
Key Differences Between Traditional Integration and FHIR
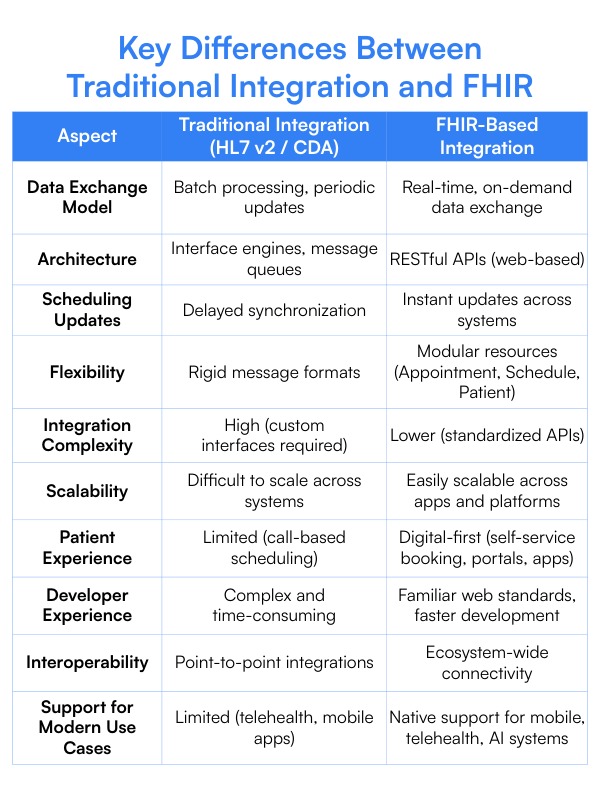
Why This Difference Matters in Real Scheduling Workflows
In a traditional setup, if a patient cancels an appointment:
- The update may take time to reflect across systems
- Front desk teams may need to manually adjust schedules
- The slot may remain unused, impacting revenue
With FHIR:
- The cancellation is updated instantly
- The slot becomes immediately available across all platforms
- It can be rebooked in real time by another patient
This shift from delayed coordination → real-time orchestration is what makes FHIR essential for modern scheduling systems.
From System-Centric to Patient-Centric Scheduling
Traditional integration models were designed around systems communicating with each other.
FHIR shifts the focus toward patient-centric experiences, where:
- Patients can book instantly
- Providers see live updates
- Systems stay synchronized automatically
This is not just a technical improvement - it’s a fundamental shift in how healthcare delivery is experienced.
How FHIR Transforms Appointment Scheduling Workflows
FHIR doesn’t just improve scheduling - it redefines how scheduling systems interact with the broader healthcare ecosystem.
1. Real-Time Visibility into Provider Availability
In traditional systems, provider schedules are often siloed within EHRs or internal tools. Updates may not reflect immediately across all platforms.
FHIR enables real-time synchronization of scheduling data across:
- EHR systems
- Patient portals
- Mobile applications
- Third-party booking platforms
This ensures that when a slot is booked, canceled, or modified, the change is reflected instantly everywhere.
The impact is significant:
- Reduced risk of double bookings
- Improved accuracy of available slots
- Faster booking experience for patients
2. Two-Way Integration Between Systems
One of the biggest limitations of older systems is one-directional data flow. For example, a patient portal may display availability but cannot update the core scheduling system directly.
FHIR enables bi-directional communication, meaning:
- Patients can book appointments directly
- Changes are written back into the EHR in real time
- Providers’ schedules are updated dynamically
This eliminates the need for manual reconciliation between systems and ensures consistency across all touchpoints.
3. Intelligent Rescheduling and Slot Optimization
Cancellations are a major contributor to lost revenue in ambulatory care.
With FHIR-enabled systems, when a patient cancels:
- The slot is immediately released
- It becomes visible to other patients in real time
- It can be automatically offered to patients on waitlists
When combined with AI (which Cabot actively supports), scheduling can go even further by:
- Predicting likely cancellations
- Suggesting optimal time slots
- Dynamically adjusting schedules based on demand
4. Automated Communication and Patient Engagement
Scheduling does not end at booking - it requires continuous communication with patients.
FHIR integrates with communication systems to enable:
- Appointment confirmations
- Reminders via SMS/email
- Pre-visit instructions
- Follow-up notifications
This reduces dependency on manual outreach and significantly improves patient adherence.
5. Enabling Self-Service Scheduling Experiences
Modern patients expect the same convenience they experience in other industries - such as booking flights or ordering services online.
FHIR makes it possible to build self-service scheduling platforms where patients can:
- Search for providers
- View real-time availability
- Book appointments instantly
- Reschedule without calling
This reduces friction and enhances the overall care experience.
Real-World Use Cases of FHIR in Scheduling
To understand the practical impact, consider how FHIR is used across different scenarios:
EHR and Scheduling System Integration
FHIR acts as a bridge between clinical and administrative systems, ensuring that patient data and appointment data remain synchronized.
Patient Portal and Mobile App Scheduling
Patients can interact with scheduling systems directly through apps, improving accessibility and reducing dependency on call centers.
Telehealth Appointment Coordination
FHIR enables seamless scheduling for virtual consultations by integrating with telehealth platforms.
Multi-Location Practice Management
Healthcare networks with multiple locations can provide unified scheduling visibility, allowing patients to choose the most convenient option.
Business Impact: What Healthcare Organizations Gain
FHIR-based scheduling delivers measurable outcomes across multiple dimensions.
Operational Efficiency
Automation reduces manual workload, allowing staff to focus on higher-value tasks.
Improved Resource Utilization
Real-time visibility ensures that provider time is used effectively, minimizing idle slots.
Revenue Optimization
Reducing no-shows and improving appointment fill rates directly impacts revenue.
Better Patient Retention
A smooth scheduling experience increases patient satisfaction and loyalty.
Measuring Success: Key Metrics That Matter
Organizations implementing FHIR-based scheduling should track:
- Reduction in no-show rates
- Increase in digital (self-service) bookings
- Decrease in call center volume
- Average time to schedule an appointment
- Provider utilization rates
These metrics provide a clear picture of both operational and financial impact.
Implementation Considerations: What It Takes to Get Started
FHIR implementation requires a thoughtful approach.
1. Understanding Current System Limitations
Organizations must evaluate their existing scheduling workflows and identify integration gaps.
2. Selecting Relevant FHIR Resources
For scheduling, key resources include:
- Appointment
- Schedule
- Patient
- Practitioner
3. Building Scalable API Infrastructure
FHIR APIs should be designed to handle real-time requests and high volumes of data exchange.
4. Ensuring Compliance and Security
Healthcare data must be protected through:
- Encryption
- Access control
- Regulatory compliance (HIPAA, PHIPA, etc.)
5. Continuous Optimization
FHIR implementation is not a one-time effort. Systems must be monitored and refined over time.
The Next Step: Combining FHIR with AI and Voice Technologies
FHIR lays the foundation for interoperability, but the next evolution lies in combining it with AI-driven automation.
As highlighted in Cabot’s capabilities:
- AI-powered voice agents can handle appointment booking
- Conversational interfaces can manage patient interactions
- Intelligent systems can optimize scheduling decisions
These advancements move healthcare toward a future where scheduling is not just digital - but intelligent and autonomous.
Conclusion: Moving Toward Connected, Patient-Centric Scheduling
Ambulatory appointment scheduling is no longer just an administrative function. It is a critical part of the patient journey and a key driver of operational success.
FHIR enables healthcare organizations to transition from:
- Fragmented systems → connected ecosystems
- Manual workflows → automated processes
- Reactive scheduling → intelligent coordination
For organizations looking to improve access, efficiency, and patient experience, modernizing scheduling with FHIR is no longer optional - it is essential.
Looking to Modernize Your Scheduling Systems?
If you're exploring how to integrate FHIR into your scheduling workflows or want to improve patient access through smarter systems, this is the right time to take the next step.
Cabot Technology Solutions brings deep expertise in:
- Healthcare interoperability
- AI-driven scheduling solutions
Let’s explore how your organization can build a more connected, efficient scheduling experience.

