The fragmentation of patient data remains one of the most persistent challenges in modern healthcare. When patients move between providers or care settings, their medical history often gets lost in the gaps, causing delays, redundant tests, and potentially dangerous errors. FHIR (Fast Healthcare Interoperability Resources), a modern standard for healthcare data exchange, is solving this problem by dramatically improving the speed and reliability of data flow across systems. At the core of FHIR are FHIR Bundles, and understanding how they work is essential for any team building or modernizing healthcare integrations.
What Is FHIR, and Why Is It Faster?
FHIR (Fast Healthcare Interoperability Resources) is an open standard developed by HL7 International for the electronic exchange of healthcare information. Unlike its predecessors, HL7 v2 and v3, FHIR was built from the ground up to use modern web technologies: RESTful APIs, JSON and XML data formats, and OAuth 2.0 security protocols.
This matters enormously for speed and efficiency.
Older HL7 v2 systems, while widely deployed (used in over 95% of U.S. healthcare organizations), rely on a rigid, pipe, delimited message structure that was designed in 1989. They are optimized for traditional, predictable workflows, admissions, lab orders, billing, but struggle with real, time data sharing and modern web or mobile integration. Every system, to, system connection is essentially a custom, point, to, point interface, making the ecosystem brittle and expensive to maintain.
FHIR changes this by replacing point, to, point interfaces with a one, to, many API model. Instead of spinning up a new custom integration for every new data exchange partner, a FHIR, compliant API can serve multiple systems simultaneously. This alone significantly reduces the time to onboard new data exchange partners. Add RESTful APIs, the same technology used by the modern web, and you get a system that is faster to implement, easier to scale, and far more interoperable across different platforms and devices, including mobile apps, wearables, and cloud, based EHRs.
In short: FHIR is faster because it is built like the modern web, not like a 1989 fax machine.
Why Is It Important to Upgrade Your System to FHIR?

The case for moving to FHIR is no longer just technical, it is regulatory, operational, and strategic.
Regulatory Mandates Are Already Here The 21st Century Cures Act and ONC's Information Blocking Rule have made FHIR API compliance non, negotiable for U.S. health systems and payers. Certified EHRs must expose FHIR "US Core" APIs covering patient demographics, medications, allergies, and more. Similarly, CMS interoperability requirements apply to Medicare and Medicaid payers. These are not future requirements, they are active obligations.
Legacy Systems Are Becoming a Liability Traditional point, to, point HL7 v2 integrations are increasingly brittle, expensive to maintain, and slow to adapt when new partners need to be onboarded. The rigid architecture of legacy HL7 v2 creates bottlenecks that modern healthcare cannot afford, and healthcare integration costs are already consuming up to 30% of IT budgets in some organizations.
FHIR Is the On, Ramp to AI and Analytics Population health analytics, ambient clinical documentation, conversational AI in healthcare, and real, time care coordination all depend on a unified, structured data backbone. FHIR provides exactly that. Organizations still running HL7 v2 in silos will find it increasingly difficult to leverage these capabilities as they mature.
Global Adoption Is Accelerating A 2025 survey found that 71% of countries already use FHIR for at least some use cases, up from 66% the prior year. The NHS in the UK, Canada's national health programs, and Australia's My Health Record are all building or expanding FHIR, based interoperability platforms. FHIR is not a future standard; it is the current direction of healthcare globally.
What Are FHIR Bundles? Individual Resources vs. Bundles Explained

FHIR breaks health data into small, individually addressable units called resources. A resource can represent a patient's demographics, a lab result, a medication, a diagnosis, an observation, essentially any discrete piece of healthcare data. Each resource can exist and be queried independently via a REST API.
But here's the key distinction: the top FHIR mechanism for real, world interoperability is not individual resources, it is Resource Bundles.
In the FHIR standard, the choice between using individual resources and Bundles depends on whether you are managing a single data point or a collection of related operations. Understanding this difference is fundamental to designing efficient, reliable FHIR integrations.
Core Differences at a Glance
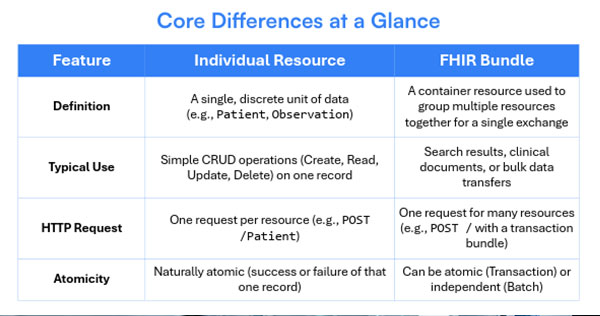
When to Use Individual Resources
Individual resources are best for granularity and simplicity. They are the building blocks of FHIR, representing specific healthcare concepts like a patient record or a lab result.
Direct Access: When you need to retrieve or update one specific record via its unique ID, for example, fetching a single patient's demographics or updating a single observation, an individual resource call is the right tool. It is clean, lightweight, and straightforward.
Decoupled Data: Ideal for systems that only need to interact with small, independent pieces of data without the overhead of a container. If your integration only needs one piece of information at a time, wrapping it in a Bundle adds unnecessary complexity.
When to Use Bundles
Bundles are essential for complex interactions and efficiency. When a clinical workflow requires multiple related resources to be exchanged, validated, and persisted together, sending them one by one creates multiple HTTP round trips, risks partial failures, and loses the relational context between them. Bundles solve all three problems in one.
Search Results: When you query a FHIR server (e.g., "find all observations for Patient X from the last 30 days"), the server always returns a searchset Bundle containing all matching resources, along with pagination links if the result set is large. Developers interact with Searchset Bundles constantly, often without realizing it, as SDK abstractions frequently hide them.
Transactions: Use a Transaction Bundle when multiple resources, a Patient, an Observation, and a Condition, for example, must all succeed or fail together as a single unit to maintain data integrity. Either every operation in the Bundle commits, or none do.
Batch Processing: Use a Batch Bundle to send multiple unrelated resources in one HTTP call to reduce network latency, even if they are allowed to fail independently. If one resource fails validation, the rest of the batch continues processing unaffected.
Clinical Documents: A FHIR Document (such as a discharge summary or referral letter) is a Bundle of type document that always begins with a Composition resource, followed by all supporting clinical data. Document Bundles are immutable, they represent a permanent, attested clinical record.
Think of it this way: a resource is like a single file; a Bundle is like a ZIP package. The ZIP contains all the files you need, preserves their relationships, and can be transmitted in one operation rather than many.
Why Bundles Win for Interoperability
The practical advantages of Bundles over individual resource calls in interoperability scenarios are significant:
Performance: A single Bundle POST avoids multiple HTTP round trips. Servers can also perform ID and reference lookups once and reuse them across all resources in the Bundle, making bulk operations substantially faster than equivalent individual calls.
Data integrity: Transaction Bundles are processed atomically, all resources succeed together or none do, preventing partial writes and clinically dangerous inconsistencies in the record.
Context preservation: Resources inside a Bundle can reference each other even before they are assigned server IDs, maintaining relational integrity across complex clinical data transfers.
Independence from containment: Unlike "contained resources", which are embedded inside a parent resource and cannot be independently accessed or modified, resources inside a Bundle retain their independent existence. They can later be accessed directly via the REST API, updated individually, or referenced from outside the Bundle.
This is what makes Bundles the primary building block for FHIR, based interoperability, not individual resources alone.
Types of FHIR Bundles and How They Are Used

FHIR defines several Bundle types, each designed for specific scenarios in clinical and operational workflows.
1. Document Bundles
Used to create formal clinical documents, discharge summaries, referral letters, care plans. The first resource in a Document Bundle must always be a Composition resource that defines the narrative and structure of the document. Document Bundles are immutable: once created, they represent a permanent, attested record of a clinical event that can be shared with external providers or archived.
2. Transaction Bundles
A Transaction Bundle groups multiple resource operations, creates, updates, deletes, into a single atomic database transaction. Either all operations succeed, or none do; if any failure occurs, the entire transaction is rolled back. This makes Transaction Bundles essential for scenarios where partial writes would create inconsistent or clinically dangerous records, such as registering a new patient alongside their initial diagnosis and medication list.
3. Message Bundles
Message Bundles implement event, driven exchange. The first resource in a Message Bundle is always a MessageHeader that describes the event (patient admission, transfer, discharge, referral, etc.). The remaining resources carry the clinical payload for that event. The sending system POSTs the Bundle to the receiving system, either synchronously or asynchronously, triggering an immediate notification and data transfer to the relevant care team.
4. Searchset Bundles
Every time a FHIR server responds to a search query, it returns a Searchset Bundle. If a clinician queries for a patient's recent lab results, the server returns a Searchset Bundle containing all matching resources with pagination links if the result set is large. Developers working with FHIR APIs interact with Searchset Bundles constantly, often without realizing it, SDK abstractions frequently hide them.
5. Batch Bundles
Batch Bundles allow multiple data operations to be sent in one request, but each operation is processed independently. If one operation fails, others continue unaffected. This makes Batch Bundles the right choice for bulk operations where partial success is acceptable, uploading multiple unrelated patient records, migrating data between systems, or running bulk updates where some records may have validation issues.
6. Collection Bundles
Collection Bundles group resources with no specific processing semantics attached. They are used for exporting patient records, aggregating data for population health analysis, or assembling data sets for migration purposes. They are the most flexible Bundle type, with the least guidance from the specification, use them deliberately and document the intended semantics clearly in your implementation.
Real, World Implementation Use Cases
Seamless Care Transitions
When a patient is discharged from a hospital, a Document Bundle can carry the complete discharge package, diagnosis, prescribed medications, treatment plan, follow, up instructions, to the next care provider in a single transfer. The receiving provider has everything they need without manually pulling records from multiple departments or making phone calls. Care continuity is preserved; administrative overhead is eliminated.
Automated Referrals
When a primary care physician refers a patient to a specialist, a Message Bundle can be automatically generated and sent at the point of referral. The Bundle includes relevant patient history, diagnostics, and the reason for referral. The specialist receives a complete clinical picture before the appointment even occurs, reducing preparation time, improving diagnostic accuracy, and eliminating the common problem of incomplete referral packets.
Medication Reconciliation Across Systems
Medication errors during care transitions are a leading cause of adverse events. A Searchset Bundle allows providers to pull a patient's complete medication history from disparate systems and reconcile it against current prescriptions, catching dangerous interactions or duplicate medications that would otherwise be invisible across fragmented records.
Bulk Data Migration and System Upgrades
When migrating patient records from a legacy HL7 v2 system to a modern FHIR, compliant platform, Batch Bundles enable bulk transfers where each resource is processed independently. Records that fail validation do not block the rest of the migration. Combined with Transaction Bundles for groups of tightly related records, this approach allows large, scale migrations to proceed efficiently while maintaining data integrity where it matters most.
Public Health Reporting
Transaction Bundles are used to submit accurate disease case reports, vaccination data, and health statistics to government health agencies. The atomic nature of the transaction ensures that reporting records are either complete or not submitted, preventing the partially, reported data that undermines public health databases and pandemic preparedness planning.
Benefits of Implementing FHIR Bundles

Faster, More Accurate Clinical Decision, Making Healthcare teams gain immediate access to complete, structured patient information. In emergency settings, this can be the difference between a rapid, informed decision and a delayed one based on incomplete data.
Fewer Medical Errors Complete medication histories, allergy records, and diagnostic context reduce the risk of misdiagnosis, duplicate prescriptions, and dangerous drug interactions, all of which commonly occur when data is fragmented across disconnected systems.
Reduced Administrative Overhead Eliminating manual data gathering, redundant test orders, and phone, based record requests frees clinical staff to focus on patient care rather than information retrieval.
Better Patient Experience Patients no longer need to re, enter their history at every provider visit or repeat tests that have already been performed. Their data follows them, seamlessly and accurately, across care settings.
Cost Savings Reducing redundant tests, administrative labor, and the maintenance costs of brittle point, to, point HL7 interfaces translates directly to lower operational costs, savings that can be reinvested in care delivery or technology improvement.
Regulatory Compliance FHIR Bundles provide the data exchange mechanism required to meet the 21st Century Cures Act, ONC Information Blocking Rule, and CMS interoperability mandates. Organizations that delay implementation face both compliance risk and growing technical debt.
Overcoming Implementation Challenges
System Compatibility Different health systems may implement FHIR slightly differently. Standardization requires ongoing collaboration with vendors and careful attention to FHIR Implementation Guides (IGs) relevant to your region, such as US Core in the United States. A middleware or integration layer that can translate between HL7 v2 and FHIR is often necessary during the transition period, allowing legacy and modern systems to coexist.
Privacy and Security FHIR Bundles frequently carry sensitive patient data, including mental health records and genomic data. Implementations must include encryption in transit, OAuth 2.0 / SMART on FHIR for access control, role, based permissions, and additional safeguards for particularly sensitive data categories.
Legacy System Migration Transitioning from legacy HL7 v2 to FHIR is not a single cutover, it is a phased process. Core HL7 v2 message types (ADT, ORM, ORU) must be mapped to equivalent FHIR resources (Patient, Encounter, Observation, MedicationRequest). Many organizations maintain hybrid environments for several years, using middleware to translate between standards while incrementally expanding their FHIR footprint. Starting with patient, facing APIs and high, value use cases (such as those mandated by the 21st Century Cures Act) allows teams to build FHIR expertise while preserving mission, critical HL7 v2 workflows.
The Path Forward
As healthcare systems continue their digital transformation, FHIR Bundles are emerging as the primary mechanism for interoperable data exchange, not because they are a mandate, but because they work. They are faster, more reliable, and more expressive than the point, to, point messaging patterns of the legacy HL7 era.
Cabot Technology Solutions helps healthcare providers and health tech teams integrate FHIR Bundles into their systems, whether they are starting fresh with a modern FHIR, native architecture or navigating a phased migration from HL7 v2. The result is a data infrastructure that is not just compliant, but genuinely capable: one where patient data flows accurately and securely across systems, care teams have the information they need when they need it, and the organization is positioned to take advantage of AI, analytics, and the next generation of healthcare technology.
The transition to FHIR is not a future consideration. It is happening now, and FHIR Resource Bundles are at the center of it.

