If you’ve been in healthcare long enough, you’ve seen plenty of technology waves arrive with big promises and then quietly flatten out.
EHRs. Portals. Population health dashboards. “Digital transformation.”
So it’s understandable if your first instinct with AI, especially generative AI is caution. You’re dealing with real patients, real clinicians, real legal and financial risk. You cannot afford to chase fads.
But 2026 is not just another “interesting” year for healthcare AI. It’s a tipping point.
- The money going into AI is real and accelerating.
- Physician and hospital adoption has jumped in a way that’s unusual for healthcare.
- The use cases around documentation, referrals, and voice based agents are finally mature enough to move the needle on time and money.
If you’re still firmly in “wait and see” mode at the end of this year, you’ll spend the rest of the decade catching up.
This article walks through why grounded in numbers and where to act first if you want AI to actually serve your clinicians and patients, not just your slide decks.
1. Why Acting in 2026 is Important

2026 is the year healthcare AI shifts from “promising” to operational—real budgets, real workflows, real expectations. Three things are happening at the same time, and together they create a tipping point.
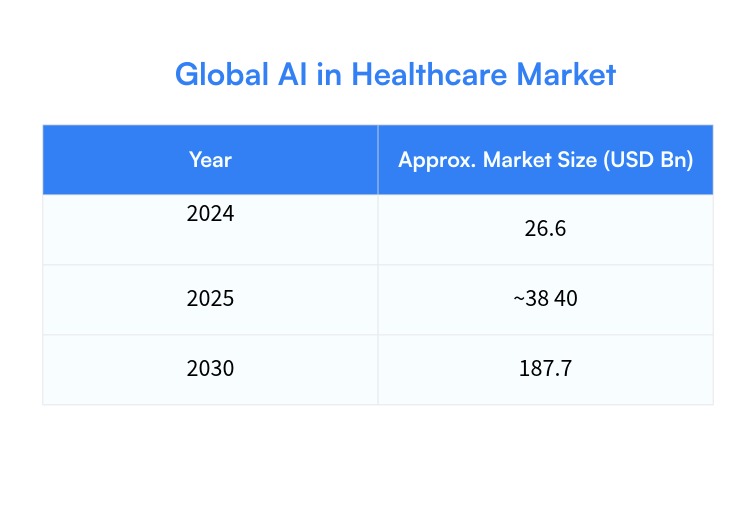
First, the money is moving. Market forecasts put global AI in healthcare at ~$26–28B in 2024, growing toward ~$180–190B by 2030 (around 38–39% CAGR). (Grand View Research) That’s not experimental spend anymore—it’s becoming a core digital investment category alongside major systems.
Chart 1 — Global AI in Healthcare Market (USD Bn)
Second, adoption is already mainstreaming. In 2024, 71% of hospitals reported using predictive AI integrated with their EHR (up from 66% in 2023), and 66% of physicians reported using AI (up from 38% one year earlier). (NCBI, American Medical Association) Even if the tools vary, the direction is clear: AI is moving into day-to-day care delivery and operations.
Third, the ROI use cases are finally mature enough to matter. Documentation support, referral orchestration, voice agents for patient calls, and operations optimization are now practical—not just demos. McKinsey and others estimate ~15% of healthcare work hours could be automated in a midpoint scenario, which translates into measurable capacity if executed well.
That’s why “wait and see” is no longer neutral. Early adopters are building compounding advantages (time returned, faster throughput, better experience). Meanwhile, if leadership delays, “shadow AI” still shows up through departments buying point tools—creating fragmentation you’ll have to clean up later.
Acting in 2026 doesn’t mean buying everything. It means choosing a few high-impact workflows, defining success in plain metrics, and putting governance + integration in place so wins can scale safely.
2. Where AI Can Delivering Real Value
There are endless AI use cases. But if your goal is to act in 2026, you should focus on four domains where the technology is proven enough, practical enough, and tightly aligned with time and money.
These are also areas where a partner like Cabot often works: documentation, referrals, voice AI agents, and operations.
2.1. Clinical documentation and ambient AI scribes
Documentation has become the tax everyone pays for digital medicine. It’s also where AI has one of the clearest near term payoffs.
Recent studies of ambient AI scribes systems that listen (with consent) and draft notes show:
- Meaningful reductions in documentation time and cognitive load. (JAMA Network)
- Decreases in measured burnout scores over just 30 days of use. (JAMA Network)
- Large health systems reporting tens of thousands of clinician hours returned in a year. (American Medical Association)
In practice, this looks like:
- The visit is recorded with clear disclosure and patient consent.
- AI turns the conversation into a structured draft (HPI, exam, plan, etc.).
- The clinician reviews, edits, and signs remaining fully responsible for the record.
This is not about replacing clinicians. It’s about freeing them from the keyboard long enough to practice the kind of medicine they were trained for.
For leadership, the benefits are concrete:
- Fewer after hours notes
- Higher quality documentation
- Better retention in specialties already under pressure
2.2. Referral management and care transitions
Almost every executive has lived through the pain of the “referral black hole”:
- Orders sent via fax, phone, or portal
- Patients waiting without updates
- Referrals that quietly stall when information is missing or capacity is unclear
AI can strengthen this chain without ripping out your existing systems:
- Classifying and prioritizing referrals based on urgency and risk.
- Checking for missing fields or attachments before the referral leaves your system.
- Orchestrating updates via SMS, email, voice, or portal, so patients and referring clinicians know where things stand.
- Highlighting stalled cases for care coordinators instead of forcing them to dig manually.
For organizations involved in post acute care, behavioral health, rehab, or multi facility networks, this is a direct lever on readmissions, no show risk, and patient satisfaction.
2.3. Voice AI agents for patient calls and reminders
Voice AI agents are maturing quickly, especially for structured, repeatable conversations:
- Outbound calls reminding patients about appointments, pre visit instructions, or medication refills.
- Inbound flows that can answer basic questions, confirm details, or route to the right team.
- Follow up check ins after discharge to catch early deterioration or confusion.
When designed well, these agents:
- Reduce staff time spent on routine calls
- Lower no show rates and last minute cancellations
- Make it easier for patients to comply with care plans, especially in high risk populations (AIPRM)
The key is to keep control and transparency: patients should know they’re talking to an AI agent, staff should be able to override and step in, and workflows must be integrated into your existing systems, not bolted on from the outside.
2.4. Operations and capacity management
On the operations side, AI is already being used to:
- Forecast admissions and ED volume
- Improve bed assignment and discharge planning
- Optimize staffing and OR scheduling (NCBI)
Even relatively modest gains a few percentage points in forecast accuracy or a small reduction in avoidable idle time translate into real financial impact when applied to large facilities and multi hospital systems.
In an environment of margin pressure and staffing shortages, these efficiencies can be the difference between reactive firefighting and proactive planning.
3. Common Traps to Avoid as You Move
Acting in 2026 doesn’t mean buying every AI product that knocks on your door. There are clear pitfalls that experienced leaders are already trying to sidestep.
3.1. Isolated AI Tools Without a Long-Term Strategy
AI tools that fix one narrow problem but don’t integrate with your data, identity, and governance layers will cause more headaches later. McKinsey’s latest healthcare AI research is explicit: organizations need to evolve from isolated point solutions to more modular architectures that can share data and orchestration. (The Washington Post)
3.2. AI that sidelines clinicians instead of supporting them
If physicians and nurses experience AI as:
- Extra clicks
- Unclear black boxes
- “Something IT pushed on us”
…adoption will stall. Their trust is the real deployment bottleneck. (Healthcare IT News)
3.3. Underestimating the data and integration effort
Voice agents, documentation tools, and referral algorithms all depend on:
- Clean interfaces into your EHR and scheduling systems
- Good identity and consent management
- Reliable logging and monitoring for safety and compliance
This isn’t “just another app.” It’s an extension of your clinical and operational nervous system.
4. A Practical Path to Adopt AI in 2026

You don’t need a perfect 10 year AI master plan. You do need deliberate moves this year.
A practical path for many providers looks like this:
Step 1 Choose a handful of high value workflows
Sit with your clinical and operational leaders and ask:
“Where are we losing the most time or money today?”
In most organizations, the same candidates show up:
- Clinical documentation
- Referrals and care coordination
- Patient access and call volume
- Bed, OR, or clinic capacity planning
Pick 3 5 areas where AI could realistically help in the next 12 18 months.
Step 2 Define success in plain language
For each workflow, decide:
- Who we’re trying to help (e.g., outpatient PCPs, hospitalists, schedulers)
- What we’re trying to change (e.g., reduce after hours documentation by 30%; cut no shows by 15%; improve time to appointment by 5 days)
- How we’ll measure it (baseline metrics + 90 day follow up)
If you can’t explain the success metric to a busy clinician in one sentence, it’s too abstract.
Step 3 Work with partners who speak both healthcare and AI
This is where a partner like Cabot matters.
You don’t just need a generic AI vendor; you need someone who:
- Understands clinical realities and regulated workflows
- Has experience with voice AI agents, referral management, and AI supported documentation
- Can integrate with EHRs, FHIR APIs, and existing digital infrastructure
- Knows how to design clinician first experiences that build trust, not resistance
Step 4 Pilot quickly, but design for scale
Start small one clinic, one specialty, one call queue but:
- Use production grade security and governance from day one
- Capture lessons and refine your AI roadmap as you go
- Think ahead: “If this works, where does it go next?”
By the end of 2026, you want to be able to say, honestly:
“We don’t just have AI pilots; we have a clear, living AI portfolio tied to our strategy and outcomes.”
5. How Cabot Fits Into This Moment
Cabot Technology Solutions positions itself not just as a software vendor, but as a healthcare AI partner for organizations that want impact, not theatrics.
Cabot focuses on:
- Voice AI agents that can call and remind patients, support front line staff, and reduce routine call volume.
- AI driven referral management, adding intelligence and visibility to transitions of care.
- Clinical documentation support, including ambient and semi structured AI tools that give clinicians time back without compromising the medical record.
For North American providers and healthtech companies, the value of a partner like Cabot is simple:
- They already understand the regulatory, workflow, and integration constraints you’re working under.
- They design AI workflows for clinicians first, so adoption isn’t an afterthought.
- They keep the focus on measurable outcomes: time saved, cost reduced, leakage prevented, experience improved.
6. 2026 as the Quiet Deadline

No regulator has circled “2026” on your calendar. But practically, this is the year where:
- Market investment is undeniable
- Adoption has crossed into majority territory
- The gap between “experimenting” and “operationalizing” is widening
You don’t need everything figured out. But you do need:
- A short list of AI relevant workflows
- A simple definition of what success looks like
- One or two trusted partners who can help you move from ideas to implemented systems
Because in a few years, your board won’t ask,
“Why didn’t we try more AI experiments?”
They’ll ask,
“Why weren’t we ready when it was obvious AI could help our clinicians, our patients, and our margins?”
2026 is your chance to start answering that question on your terms, with clear priorities, and with partners who understand healthcare as deeply as they understand AI.

